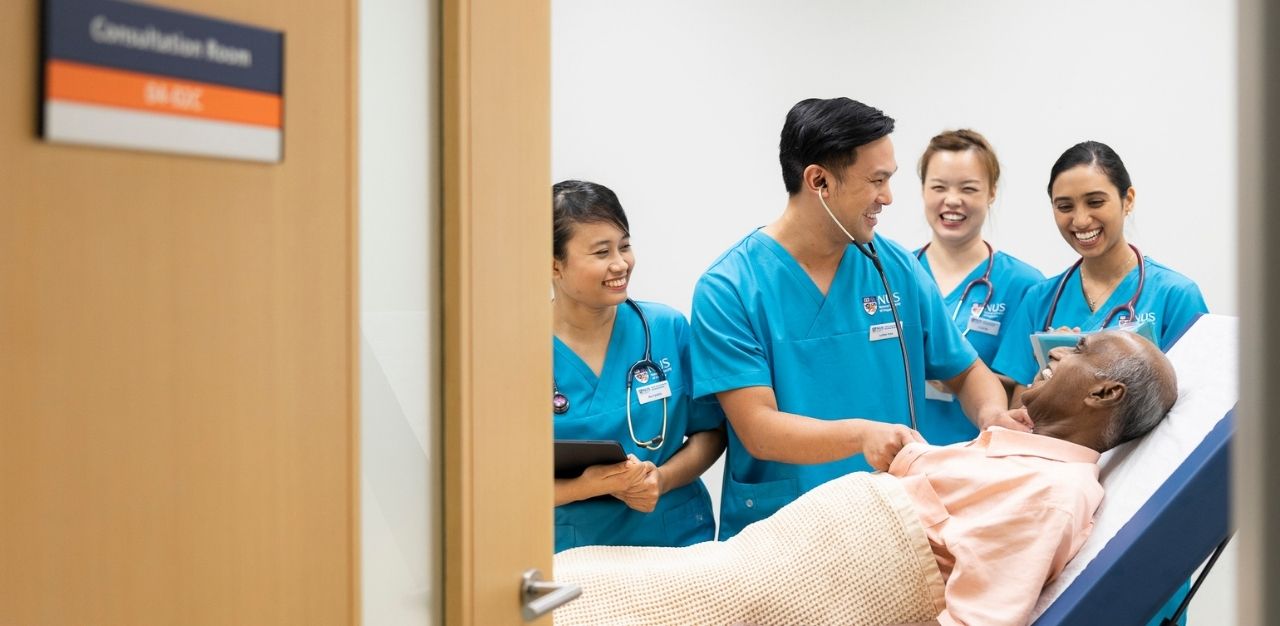
The days where one might witness nurses following doctors around wards on their rounds may well be over. Luther Yiew, an Assistant Nurse Clinician at KK Women’s & Children’s Hospital, believes that this “role blur” taking place among healthcare teams now represents the future of the healthcare landscape.
In July 2021, Health Minister Ong Ye Kung announced that the Singaporean government hopes to have by 2030 up to 700 Advanced Practice Nurses (APNs) in Singapore who are licensed to prescribe medication for patients.
Through the National Collaborative Prescribing Programme (NCPP) established in 2018, APNs and pharmacists can now earn prescribing rights through holistic training. Currently, out of 294 APNs, 57 APNs already have prescribing rights – and the goal is to have 400 more by 2030.
Little public awareness of changing nursing scene
Despite these progressions, the layperson Singaporean has yet to fully grasp the full scope of the nursing profession today.
“According to my research, even patients who are highly educated have little understanding of what an APN is,” says Dr Brigette Woo, research fellow at NUS Alice Lee Centre for Nursing Studies (NUS Nursing) who is undertaking research on APNs. “Many have the conventional mindset that nurses only do simple tasks like measuring a patient’s blood pressure.”
She explains that this might be due to the public only observing nurses performing very basic skills and carrying out menial tasks, which is merely a tiny component of what nurses do today.
Dr Chong Yap Seng, Obstetrician and Dean of NUS Yong Loo Lin School of Medicine, adds that APNs are often confused with other medical professionals by the public. “When people visit family clinics, they might think that they are observing nurses assisting doctors, but they are actually clinical assistants. Nurses have higher qualifications these days,” he says.
Even patients who might have been seeing APNs for an entire year may have thought that they were seeing a doctor the entire time, according to Dr Woo’s study.

This lack of public awareness might seem inconsequential, but are directly felt by those who pursue nursing as a profession at one point or another.
“During an open house, one of my ex-students came with his parents and he addressed me as ‘Dr Shefaly’. I remember having to explain to his confused parents for the next 15 minutes how nurses can also do PhDs,” says Dr Shefaly Shorey, Assistant Professor at the NUS Nursing. “It’s still hard for people to understand that nurses can also be ‘doctors’.”
She shares that it is not uncommon for the public to think of nursing as the option students take when their grades aren’t good enough, and they have no other course to take, even though that is often far from the truth.
For her, nursing was a calling. She saw how her terminally-ill grandmother-in-law was provided holistic care by the nurses. “They made a huge impact on me, because I noticed that despite all the pain she was going through, she would be very grateful to the nurses and give blessings to them,” says Dr Shefaly.
She made a mid-career switch from teaching into nursing and has never looked back.
This was also the case for Dr Zhou Wentao, an APN and Programme Director of the Master of Nursing Programme at NUS Nursing. After entering medical school in China and accepting a Ministry of Health scholarship in her first year, Dr Zhou came to Singapore to pursue nursing.
Her mother, who was a doctor, wasn’t thrilled by the idea at first.
“Although she had reservations about me taking up nursing, she was reminded of the Chinese idiom, ‘a person’s healing process is 30 per cent treatment and 70 per cent care’, so she agreed to me taking up nursing eventually,” she shares.
Far from being a “backup choice”, Dr Woo believes that it takes copious amounts of resilience to become a nurse.
“I always tell my students that if they don’t have the passion for nursing, then they really need to think twice about pursuing this career path,” she says. “Passion is the one thing that drives our work, and I wouldn’t want any Tom, Dick, or Harry to join our industry either.”
“Medicine is also a tough job, but doctors receive recognition and respect. As a nurse, you can be doing a lot of things under the radar, and you don’t get celebrated, acknowledged, or even properly remunerated at times,” she added.
Remnants of the stigma against male nursing still exist
This stigma can sometimes be conflated with the outdated notion that nursing is a female profession. Mr Yiew, who is also the first male nurse to work in KKH’s wards, shares that KKH previously only allowed male nurses to work in the children’s ICU, operating theatre and children’s emergency wards.
“They initially thought that by confining male nurses to certain care contexts, it would be more advantageous to us,” he says. “But I think that restricted some of us who were interested in nursing children in [regular] wards, like myself.”
Thanks to his self-advocacy, Mr Yiew’s male juniors can now exercise the same vocational options as their female counterparts.
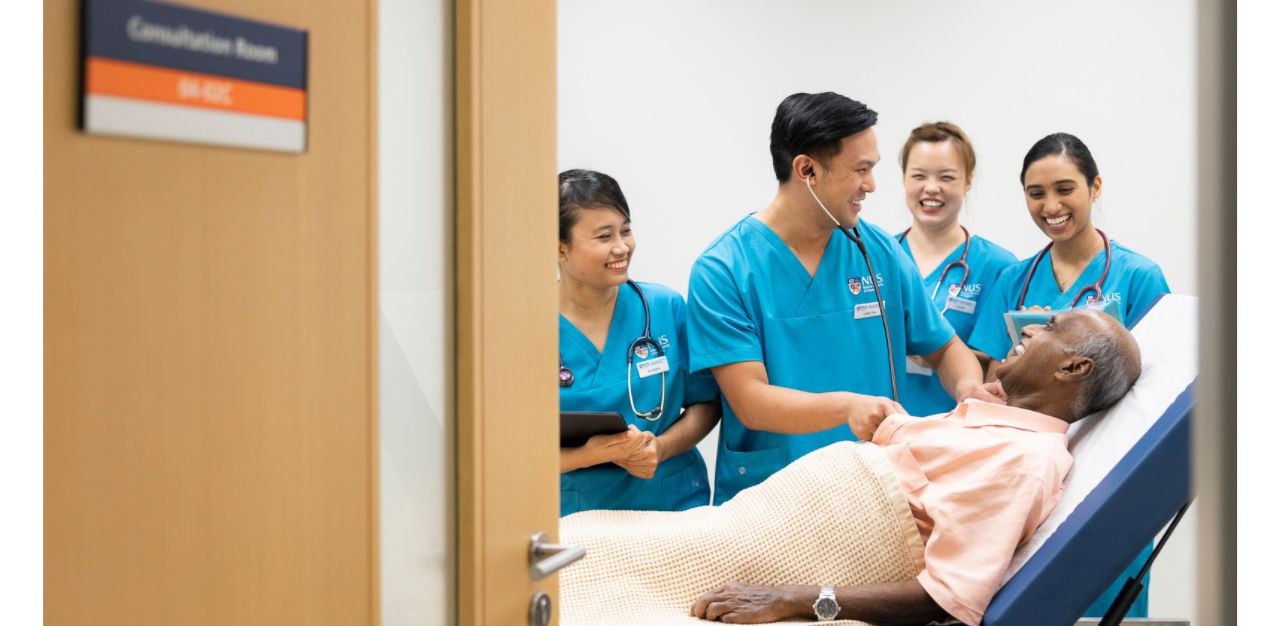
Mr Yiew is currently pursuing a Master of Nursing degree, which will make him the first male APN at KKH.
“I think some members of the public are apprehensive about the care provided by male nurses,” he says. “This is why we conduct ourselves professionally and make sure that we uphold our profession and have flawless standards of care.”
Mr Yiew is currently one of the 15 nurses in a hospital with more than 1,800 nurses, but he believes that the novelty puts him at an advantage. Many a time, it works as a great conversation starter and gives him an entry into better patient interaction.
“In terms of direct care, it doesn’t impede us – in fact, it empowers us,” he says. “When I nurse male teenagers or children who need an invasive procedure like inserting a suppository, they often prefer that I do it for them because I’m a fellow male, so it’s less uncomfortable.”
Dr Zhou believes that patients’ receptivity towards nurses is a matter of personal preference. “A female patient might prefer a male nurse to take care of her because of his caring nature, and vice versa. We need to look beyond stereotyping nurses by gender,” she adds.
Similarly, at the end of the day, joining nursing is a personal preference and calling. “Regardless of care context, we will always need both high-quality male and female nurses to complement patients’ needs,” she says. Some care contexts such as disaster care might even require more male nurses.
Currently, 11 per cent of the registered nurse population is male, but that number is steadily rising thanks to the likes of Mr Yiew, who proudly channelled his aptitude for care into his profession.
“It was through my undergraduate studies that I realised my flair for giving children comfort, as well as having their parents instil confidence in my care. I realised that was something very worthwhile to me,” he shares.
Having been brought up in a family of engineers, Mr Yiew’s parents were initially hesitant. But as he started providing care for their chronic ailment, his vocation became something they started to see value in and gradually support.
Changing public perceptions
Moving forward, Dr Zhou emphasises that nurses themselves need to promote themselves more holistically to the general public, by redefining their roles and revaluing their work based on their patients’ recovery journeys.
“My students sometimes get bothered by the fact that society is unaware of the full scope of the nursing profession,” says Dr Shefaly. “I would like to believe that this is changing, but if people still approach me on the issue, I’ll see it as a wonderful opportunity for me to educate my fellow Singaporeans on what we nurses do.”
Find out more about the scope of responsibilities nurses have in the latter of this two-part series: No longer just handmaidens to doctors: Nurses take on more leadership roles.
Join the conversations on TheHomeGround Asia’s Facebook and Instagram, and get the latest updates via Telegram.