Theirs is a calling to help others. They are frequently drawn towards giving care 24/7, helping to alleviate the pain and suffering of their charges, sometimes even shouldering grief and depression — to the point where they set aside their own mental and physical health.
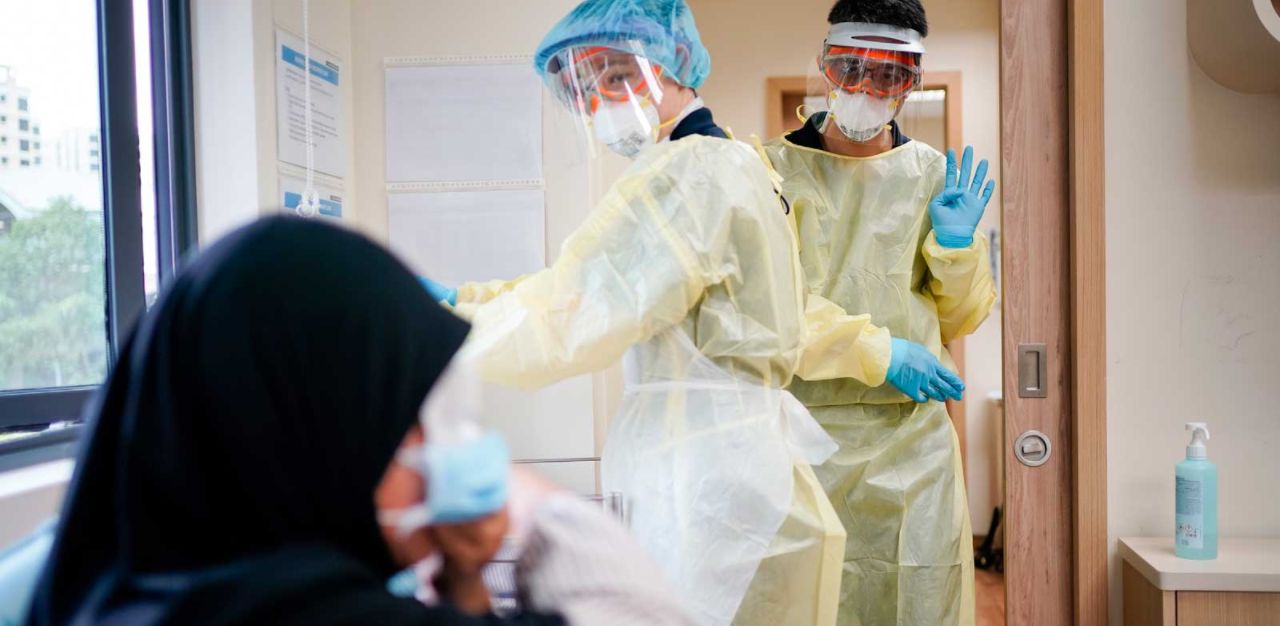
So, what happens when you have to give so much, and are told it is still not enough?
What is compassion fatigue?
With the prolonged Covid-19 pandemic and the restrictions imposed by governments, many people are now hardened by compassion fatigue. Compassion fatigue, or sometimes referred to as empathy burnout, can occur for anyone working with individuals who are experiencing physical or emotional stress. It is a normal result of chronic stress from caring for those we feel compassion for.
As a form of secondary traumatic stress, compassion fatigue is an occupational hazard faced by many working in environments where they are subjected to other people’s trauma over prolonged periods of time. The nature of traumatic exposure might be indirect, but secondary traumatic stress can trigger symptoms as serious as those associated with Post-Traumatic Stress Disorder (PTSD), such as intrusive imagery, distressing emotions, and cognitive changes.
Signs of compassion fatigue may include physical and emotional exhaustion, increased anxiety, sadness, anger, irritability, feelings of helplessness in the face of patient suffering, reduced feelings of empathy and sensitivity, physical symptoms like sleep and appetite disturbances, and a diminished sense of purpose.
Compassion fatigue is often conflated with burnout, which is associated with everyday stressors in the workplace, while the former is related to what care professionals absorb from their patients. According to psychologist Heidi Allespach, PhD, of the University of Miami’s Miller School of Medicine, they can become “so over-empathetic that they find themselves growing numb to their patients’ suffering”. However, the two often go hand-in-hand.
This phenomenon is mostly observed among professionals who work in a “healing or helping capacity” — thus, legal and medical professionals, therapists, first responders, nurses, and service providers of any kind are most at risk for developing compassion fatigue.
First-responder: Trauma, guilt, and self-blame

“If anything happens to him, I’m going to sue you.”
This is what Benjamin, 24, has heard on more than one occasion throughout his two-year attachment as a paramedic. He had attended to many cardiac arrest cases where patients remained unresponsive, and panic-stricken family members would hurled verbal abuse at him in the face of their grief. “Why is he not responding?” they would accuse. “You must be doing something wrong.”
“Scenarios like this were quite common… I’d try my best to calm them down. I understood how the families were feeling, so I didn’t blame them, but it made me feel even more helpless in a situation already beyond my control,” Benjamin, who would prefer to stay anonymous, says. “Under certain circumstances, we need to send patients to a hospital further away because not all hospitals can take in every kind of patient, like burn victims or infant cases. In these situations, the family members get very upset. It is understandable — but there’s nothing we can do about it.”
The Covid-19 pandemic also introduced new challenges to the job. That was when the protocol called for first-responders to be outfitted with full Personal Protective Equipment (PPE) on every dispatch. Benjamin recalls hiking through Bukit Timah Nature Reserve in full PPE gear in the heavy rain to attend to a woman with a sprained ankle and was unable to walk. “Every call is unforgettable,” he says. “But I know [helping people] is just something I’ve always wanted to do.”
His voice takes on a more sombre tone as he recounts the time he failed to resuscitate an infant, who was beyond saving. This is just one example of the countless traumatic experiences he had experienced on the job. He admits that it was deeply distressing to bear witness to so many horrifying events, especially at the beginning.
It is a painful and near-impossible feat to remove yourself from the situation, and he feels a sense of guilt and responsibility for every patient he was unable to save. “After a while, you force yourself to become desensitised,” he says. “You do get so-called ‘used to it’, but of course, these things will still stick in your mind for a very long time.”
Caregiver to a loved one: Feeling alone, afraid, and frustrated
As President Halimah Yacob highlighted, being a caregiver to a family member who is sick means that you are “on call” nearly “all day” — a full-time job that is often overlooked for its intense load of responsibilities and the overwhelming emotional burden that comes with it.
For family caregivers, compassion fatigue can be an extreme state of tension and stress that results in feelings of hopelessness, indifference, and pessimism.

While most caregivers are middle-aged, Sadie was only 21 when she was a caregiver to her ailing grandmother. She was then pursuing her full-time diploma studies and taking turns with her mother who was also juggling a full-time job.
When her grandmother was hospitalised, Sadie, who did not want to give her full name, not only fed and washed her, she also changed her stoma bag, and assisted with her physical therapy. When her condition deteriorated, Sadie was involved in the complicated process of tube-feeding, cleaning, and diaper-changing.
Whenever the nurses could not attend to her grandmother as quickly as she would have liked, Sadie would feel anxious despite understanding that the hospital staff were being pushed to their limits and trying their best.
“The elderly can get very sensitive. My grandma would throw tantrums like a child,” Sadie recalls. “When she had to get her needle changed for her IV drip, she would forcefully stop the nurse from helping her. We both spent a long time consoling and appeasing her.”
Bringing her grandmother home was also an arduous process. Sadie and her mother had to make arrangements for a special bed and commode, and get acquainted with medical apparatus and medication. They were trained by the hospital. Taking her grandmother to the polyclinic for check-ups was equally stressful. They had to plan and strategise on which wheelchair-friendly routes to take to ensure she was comfortable.
Anticipating the turns in her grandmother’s condition was an unending emotional roller coaster, and Sadie persisted through many turbulent and lonely nights where she felt guilty for taking any rest or having to manage her studies. Apart from grappling with her own fears of getting old, falling ill, and facing death, she was also wracked with feelings of powerlessness whenever she tried to take away her grandmother’s pain.
“Yes, there were a lot of challenges,” she says. “But the biggest one came when it ended. I fell into a bigger grief, and I still wish I had given her even more love and support.”
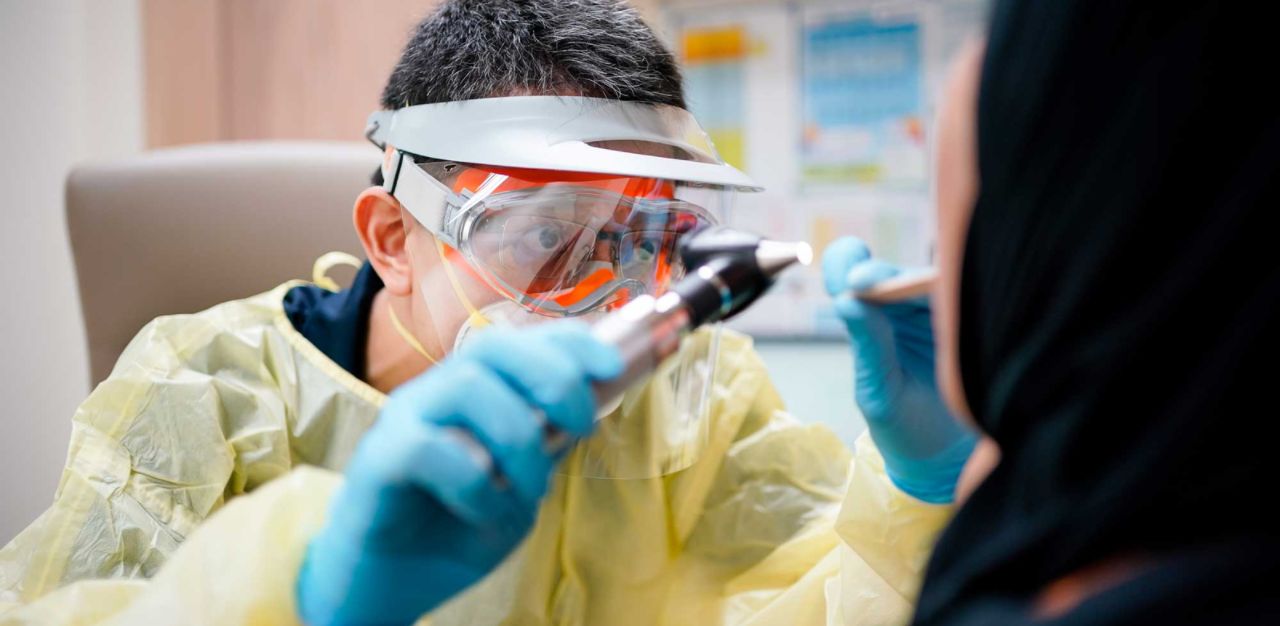
What can be done to help care professionals
The stressors of working in a care profession have been drastically compounded by the pandemic, which also resulted in a widespread mental health crisis. Our healthcare sector has taken the hardest hit, as demonstrated by the mass exodus of nurses in recent months. Singapore’s frontline workers have been stretched thin as they continue to soldier on with no end in sight.
To alleviate their burden, the government has implemented support like mobilising healthcare volunteer corps and the Singapore Armed Forces (SAF) to address the manpower shortage, and allowing public healthcare staff to utilise hospitalisation leave instead of outpatient sick leave when they are unwell.
However, anonymous healthcare workers have turned to social media to share their responses and draw attention to the grim situation on the ground.
“I’m just really disappointed because it’s not about recruiting more people. … It’s about really caring for your staff,” one of them posted. “It’s about really taking the time to understand what their needs are and making the necessary changes. Covid-19 didn’t create the problems. It just surfaced the problems that were already there for the longest time.”
By improving policies and having a systemic prevention programme in place, it would perhaps protect and empower them to care for themselves and their patients in a sustainable way. The healthcare institutions should also build a healthy work environment, advocate for self-care, and provide organisational support to encourage staff to voice out should they need help. This can include increasing access to resources, such as free psychological services and community initiatives.
A spokesman for the Medical Protection Society, which lends support to 5,000 healthcare professionals in Singapore and has offered confidential counselling services to its members since 2020, affirms that more can be done by focusing on “providing easier access to the right kind of support, which can help medical professionals to manage specific issues discreetly and continue to perform at their best”.
Both the Singapore Psychiatric Association and Singapore Medical Association have also provided numerous support services, like pro bono psychological counselling.
For caregivers at home whose stressors have also been exacerbated by the pandemic, additional support is provided in helping them transition more smoothly from the hospital. For one, Tan Tock Seng Hospital (TTSH) Nursing started Carer Matters, a programme providing holistic assistance for caregivers following the discharge of their loved one from the hospital. This includes educational programmes and personalised resources, help in sourcing for services and grants, and invaluable emotional support.
Kindness makes the world a kinder place
Like healthcare personnel all over the world, healthcare workers in Singapore are also overburdened and stressed out, working gruelling hours with little time for breaks, be it for food, rest, or even using the bathroom.
As frustrated as everyone may feel under the straining healthcare system, it is often disheartening to hear stories of people lashing out at healthcare workers over long waiting times or when staff have too much on their plate to provide immediate non-urgent assistance or information. By being responsible and understanding, we can also do our part in alleviating their day-to-day stress.
While care professionals play a critical role in aiding the recovery of others, they too have needs and face mental and physical challenges, especially in these tumultuous times.
Join the conversations on TheHomeGround Asia’s Facebook and Instagram, and get the latest updates via Telegram.















Thanks for sharing. I read many of your blog posts, cool, your blog is very good. https://www.binance.info/register?ref=IXBIAFVY
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.